November is National Osteoporosis Awareness Month and the good news is that keeping our bones healthy is possible throughout a range of nutritional and lifestyle factors.
According to the International Osteoporosis Foundation, osteoporosis and low bone mass affects approximately 44 million women and men over the age of 50 (and even younger) which is why problems associated with low bone mass are now said to be a major public health concern.
What is Osteoporosis?
Osteoporosis is defined as “a bone disease that occurs when the body loses too much bone, makes too little bone, or both.”
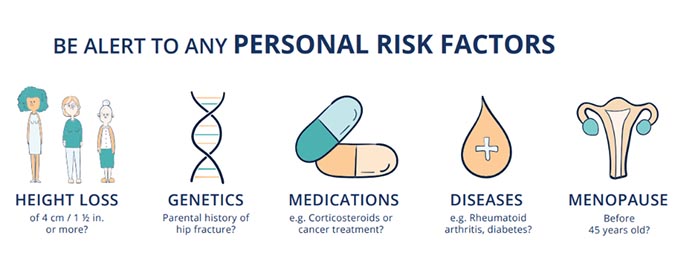
Osteoporosis Causes & Risk Factors
Low bone mass is usually caused by a combination of factors, typically including older age, nutrient deficiencies due to eating a poor diet, existing health conditions and others. The main causes of osteoporosis include:
- Inactivity or too little exercise which helps to maintain bone mass
- Aging
- Hormonal changes and imbalances, especially low estrogen levels in women, which is the cause of many menopause symptoms. Low levels of testosterone in men can also decrease bone mass. Women suffer from osteoporosis more than men largely because of a decrease in hormones after menopause.
- History of medical conditions such as autoimmune disorders, pulmonary disease, kidney or liver diseases
- Long-term use of certain medications, including proton pump inhibitors (PPIs), selective serotonin reuptake inhibitors (SSRIs), aromatase inhibitors, fertility drugs/hormonal medications, anti-seizure medications and steroids (glucocorticoids or corticosteroids).
- Low vitamin D levels
- Nutritional deficiencies, especially in vitamins and minerals that help to build bone such as calcium, phosphorus and vitamin K
- Weight loss dieting that results in severe calorie restriction and malnutrition
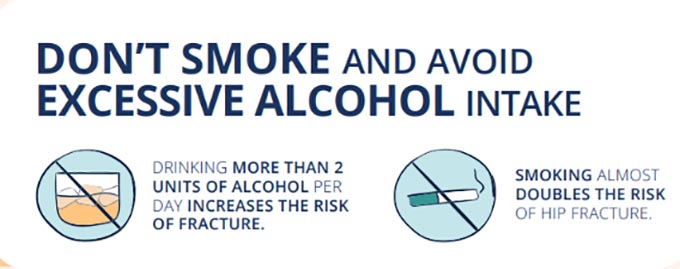
Additional risk factors for this condition include being smaller or thinner than average, smoking and drinking excessively, and having a family history of osteoporosis.

Nutritional and lifestyle strategies:
- Natural osteoporosis treatments that can be highly effective include getting enough exercise such as walking, yoga, pilates, swimming, functional body movements, trampolining and especially doing resistance and strength training 2 to 3 times weekly.
- Other areas include treating hormonal imbalances, preventing Vitamin D deficiency and eating an an anti-inflammatory diet can all be addressed. Your diet can play a critical role in your bone health because it determines if you’re obtaining enough protein and essential vitamins and minerals — especially calcium, magnesium, phosphorus, boron, omega 3 and manganese that all play a role in bone formation.
Below are some general guidelines on NUTRIENTS to focus on however, a personalized approach is recommended for each individual as we are all at different ages and stages of life with different needs.

Protein
Protein makes up about 50% of your bone volume and ⅓ of your bone mass, so taking in optimal amounts of protein on a daily basis is incredibly important for bone health. Studies show that suboptimal protein intake increases the risk for low bone mineral density and that older adults following higher protein diets tend to have higher bone mineral density and lower fracture risk.Because of this, some osteoporosis experts recommend a protein intake between 1.0–1.2 grams per kg (.45-.54 grams per pound) per day, which is much higher than the current Recommended Dietary Allowance (RDA) of .8 grams per kg of body weight (0.36 grams per pound).
- Seafood: Emphasize omega-3-rich varieties such as wild Alaskan salmon, herring, anchovies, sardines, and cooked oysters.
- Poultry: Enjoy chicken, duck, quail, and cornish hens and consume with the skin and fat.
- Meat : lamb and beef – consume with fat and avoid over cooking
- Eggs: Consume eggs from pastured hens whenever possible.
Dairy
Eat full-fat, organic unpasteurized dairy if tolerated (milk, yogurt, cheese) from grass fed cows as well as other cheeses including feta, goat, sheep and kefir). Dairy can be a good source of calcium if digested however, I have compiled a comprehensive list of calcium and magnesium rich plant foods to include in your diet. Get it here >
Healthy Fats
Essential for nutrient absorption, adequate fat enhances the absorption of the key fat soluble vitamins, D and K2, as well as the minerals, starting with calcium, that contribute to bone strength. Healthy choices include:
- Oils/Butters: Coconut oil, coconut milk, extra virgin olive oil, avocado oil, butter and ghee
- Avocado: Avocado are a source of healthful fatty acids and nutrients.
- Olives: Extra virgin olive oil and olives (up to 4 – 5 daily) contain important trace minerals.
- Nuts: Nuts are a healthy and rich source of proteins and good fats.
Vegetables
Vegetables provide necessary minerals and phytonutrients. Eat vegetables lightly steamed or raw in salads with olive oil and apple cider vinegar dressing.
Fermented Foods
Naturally fermented foods enhance digestion and immune function as well as providing valuable vitamin K2. Choose from sauerkraut,kimchi, fermented pickles, cultured vegetables, miso and kefir.
Celtic Sea Salt
This provides valuable trace minerals as a salt to taste.
Prunes!
Prunes, specifically, have a potent effect on reversing bone loss, demonstrated in increased bone density, and increased percentage of weight-bearing trabecular bone.
Foods to Avoid
- Sodas: Sodas of all sorts can interfere with healthy bone physiology and are not a beverage of choice
- Sugar: Limit sugars as needed to keep a healthy weight and metabolism.
- Alcohol: Avoid excessive alcohol consumption.
- Low-fat, nonfat, or pasteurized dairy products: These highly processed foods do not enhance calcium or vitamin absorption.
Marsha Fenwick, C.N.P. R.R.T.
Marsha is not your typical nutritionist. She began her career 20 years ago as a Registered Respiratory Therapist. Later, she earned her certifications as a Registered Nutritional Consultant Practitioner, Certified Nutritional Practitioner, and Registered Orthomolecular Health Practitioner. Marsha is also a Certified Cancer Coach. Her clinical practice specializes in: sustainable healthy weight loss, digestive health, women's hormones, diabetes, heart health, and cancer prevention and recovery. Contact Marsha today for more information and to book a FREE 15 minute nutritional consultation.